When the Medication Changes Everything:
What Antidepressants Can Do to a Relationship
Thousands of people describe the same experience: a loving partner starts taking an
antidepressant, and within weeks, the person they knew is gone. What is happening
— and why isn’t anyone talking about it?
It usually starts with a small shift. A little more distance. Fewer texts during the day. Eyes tha
don’t quite meet yours the same way. Then, sometimes very quickly, something ruptures.The person you have shared years with — your partner, your spouse, the parent of your children —
sits across from you and says words that feel impossible:
“It blows my mind how much all of the verbiage is almost exactly the
same. Almost every time.”
I don’t love you anymore. I’m not sure I
ever did. I need to leave.
In an online support group that has attracted thousands of members, people from around the world
have documented this same pattern, over and over, with an eerie consistency. The common thread:
one partner recently started, changed, or stopped taking an antidepressant — typically an SSRI or
SNRI. There is a real, documented phenomenon that the medical system has been
slow to acknowledge: these drugs can profoundly alter personality, emotion, and intimate
attachment — sometimes in ways that destroy relationships and leave families in pieces.
When doctors prescribe antidepressants, they typically discuss the common side effects — nausea,
insomnia, sexual dysfunction, weight changes. What they rarely mention is a cluster of effects on
emotional life itself. These are not side effects in the trivial sense. They can fundamentally alter how
a person feels about everything and everyone they love.
| Symptom | What it means for Relationships |
| Emotional Blunting | A flatness or numbness that mutes both negative and positive feelings — including love, joy, and empathy. Partners report feeling like they are living with a stranger. |
| Anhedonia | Loss of pleasure in things that once brought happiness — family, intimacy, hobbies, connection. The medicated person may describe life as hollow or pointless. |
| Depersonalization | A dissociative state in which the person feels detached from themselves and their life. Decisions made in this state can seem irrational or unrecognizable to everyone who knows them. |
| Sexual Dysfunction | Reduced libido, difficulty with arousal or orgasm. This can persist long after stopping the medication (a condition called PSSD), causing lasting strain on intimacy. |
| Medication Induced Mania | Impulsivity, grandiosity, affairs, reckless spending, rage, and sleeplessness — especially in those with underlying bipolar vulnerability. Often triggers a misdiagnosis of bipolar disorder. |
| Withdrawal Stabilization | Coming off these drugs — even gradually — can trigger severe psychological instability lasting weeks to months: rage, mania, deep depression, dissociation, and personality changes. |
The Light Switch Moment
Partners who discover this connection almost universally describe a moment of sudden recognition
— when the timeline clicks into place. They look back and realize: the coldness started within
weeks of the new prescription. The mania began days after the dosage increase. The personality
came back during the week the medication ran out.A couple weeks after she left, she ran out of her meds. That week she didn’t
have them, she was caring, loving, attentive, sweet. She was my wife. Then
she told me she hadn’t been on her meds that week and it just clicked.
Everything made so much sense.”
The Misdiagnosis Cycle
A particularly troubling pattern appears repeatedly in these accounts: a person starts an
antidepressant, develops manic or psychotic symptoms as a result, and is then diagnosed with
bipolar disorder — a diagnosis that leads to more medications, more instability, and a longer, more
chaotic unraveling. In several documented cases, people who were given bipolar diagnoses during or after SSRI use
were later retested and found to have no underlying psychiatric disorder at all. The mania was
drug-induced. But by then, years of additional medication had compounded the damage.
“I have been saying for years that I should write a book. I nearly lost my
— Former SSRI and Lamictal user, now off all medication
whole world. I was retested by a different psychologist and the tests found
no psychopathology — no bipolar, no depression, nothing. The ‘happy pills’
made me so happy I didn’t care about anything. My kids now call that
period ‘the summer from hell.’
What the research suggests:
SSRIs and SNRIs are known to trigger
manic episodes in people with bipolar vulnerability — sometimes revealing
a diagnosis that wasn’t apparent before. But they can also induce mania in
people without any pre-existing condition. When mania is treated as an
underlying disorder rather than a drug effect, patients often receive
additional medications that cause further destabilization. Clinicians and
patients alike benefit from asking: did this begin with a medication change?
The medicated person’s experience
It would be easy to cast these stories as the medicated partner being the villain. That misses
something important. Many people on antidepressants do not know what is happening to them.
From inside the numbness, they cannot feel what they’ve lost. The emotional blunting that erases
their love for their partner also erases their ability to perceive the intoxication anosognosia.
I was put on pills very young. Every time I stopped taking them or changed
them, they really did change my personality — a mental health crisis,
spiritual crisis, relationship crisis altogether in one. I’m sorry for the hurt I
caused to others. I also hope that others can understand how much it hurts
for me to go through all of this too.”
— Person medicated from age 16
“None of them — not the therapists, the psychiatrist, or any of the
Tweet
doctors — ever suggested that the medications could be contributing
to these drastic changes. It was this group that finally brought that to
light.”
For the unmedicated partners, the hardest part is often invisibility. They watch their marriage
collapse, they try to explain to professionals that something has changed, and they are dismissed —
or worse, cast as the controlling or abusive one by a partner whose perception has been chemically
distorted.
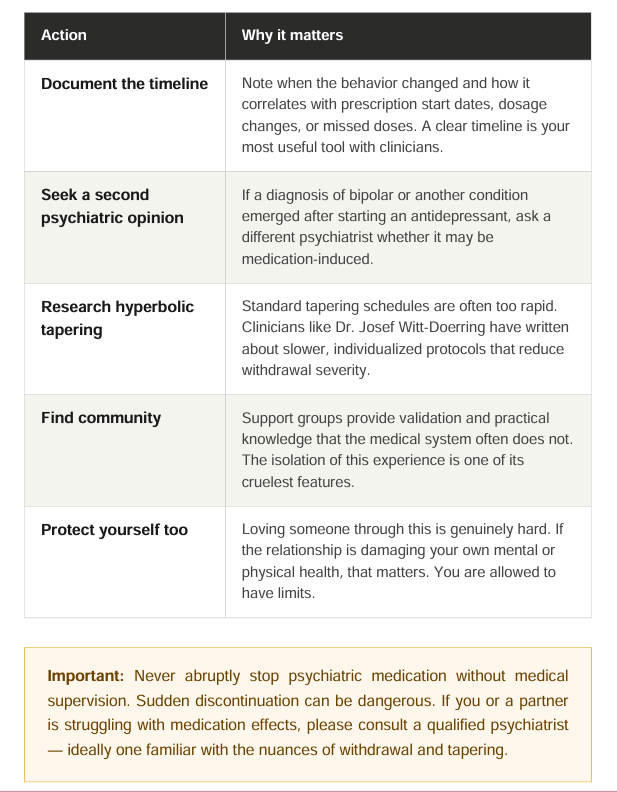
What You Can do
If you recognize your situation in these accounts, here are some steps that others have found
meaningful
The Stories That Don’t Get Told
Prescription rates for antidepressants have risen dramatically over the past two decades. Millions of
people are on these drugs, and the vast majority will never connect their medication to a relationship
collapse — because the connection is rarely surfaced by the people prescribing them.
The people who find their way to support groups are the ones who went looking. They are not a
statistical sample. But their stories — told independently, from different countries, across different
years, describing the same symptoms, the same phrases, the same light-switch moments —
constitute something worth paying attention to.
Antidepressants help many people. They also, in ways that are poorly understood and poorly
communicated, sometimes dismantle the emotional life of the person taking them — and in doing
so, dismantle everything those emotions held together.
That is worth knowing before you fill the prescription.

